What can be done right now to save NHS General Practice, in a form that is works for patients, practice staff and taxpayers? What should the new Health Secretary Therese Coffey do about GP access?
First of all she needs to understand what GPs do.
The motto of the Royal College of General Practitioners is Caritas cum Scientia

When politicians and journalists talk about general practice they give the impression that they think GPs see two kinds of patients; those with simple problems that they can fix and those with more complicated problems that need to see a specialist. They seem to think that someone else should be able to sort out the simple problems and perhaps patients should be able to go straight to a specialist. Sometimes I think they cannot quite see the point of GPs. The reality is that on average about 1 in 10 patients are referred, about 2 in 10 are straightforward and the rest are suffering with long-term, intractable problems like chronic pain and chronic anxiety and depression compounded by a range of complex social circumstances and physical illnesses.
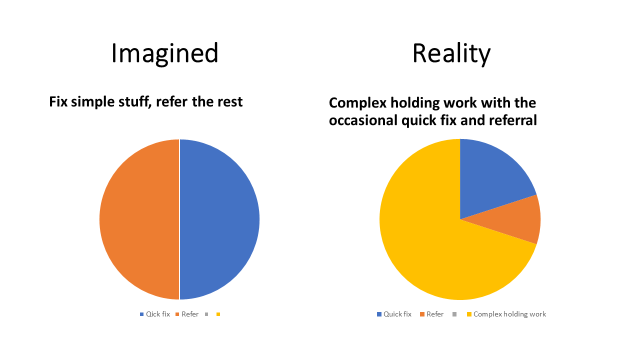
More often than not GPs provide holding work, care and presence in the face of enduring, intolerable suffering. The relationships are where the medicine happens, the GPs are the theraputic agents
So what needs to happen to save NHS General Practice? What should the new Secretary for Health, Thérèse Coffey do now?
1.Access to GPs is best when the right person helps patients at the right time. This depends on excellent clinical and administrative triage from people who know the patients, the practice and the community. Since introducing this at my practice, we have continued to ensure continuity of care at the same time as enabling every patient who contacts the practice an appointment within 2-3 days.
2. Access to GPs is best where health needs are least because the wealthiest areas tend to have the healthiest people and more GPs. Access to GPs is worst where health needs are greatest because these are the most deprived and under-doctored areas. She needs to match funding to need.
3. Good access depends on good management. There’s no reason why the NHS shouldn’t have the best healthcare managers in the world. She should invest in primary care management including finance and HR, within practices and at scale.
4. Of all the new clinical roles in primary clinical pharmacists and pharmacy technicians based in practices are most valuable and these roles should be supported. There is little evidence to show that other new clinical staff can provide support at the scale needed. Undoubtedly there needs to be more investment in practice nurses and District nurses.
5. Continuity of care underpins every aspect of quality, safety and experience in primary are. She should support all measures being promoted by the Royal College of GPs to improve continuity including organisational incentives and public education.
6. She should do everything possible to retain GPs who already have long-term relationships with patients and practices because thousands of them are retiring early, reducing their hours or pursuing other work because the conditions they are working in are too stressful.
7. Satisfaction for patients and GPs is being undermined by a relentless focus on measurement, scrutiny and incentives, so that hours every day are spent collecting data that is of little use to patients or their GPs. She should reduce this as far as possible by following the advice of Don Berwick who the conservative government invited to review quality and safety in the NHS in 2013.
It’s tempting to set targets like seeing patients face to face within 2 weeks but if there are too few staff and the ones that remain are miserable and exhausted then targets like this will only worsen the problem of burnout and GPs leaving. General Practice can be and should be full of joy amidst the suffering and there are still GPs who love their job, but there could be many more, and the government can help with this today.

Once again, you make sense. Will the measurers listen? I hope so, but fear they will carry on missing the relationships where the uncountable holds the value.
Thank you!
Excellent article. Seeing new patients for short triaging type encounters, one problem at a visit, is a waste of my skills. The patients don’t have time to learn to trust me and work with me. Complex cases cannot be sorted out, thus I end up either dealing with simple conditions (which nurses or clinical pharmacists could see) , or referring the patients on to specialists, often because the patients won’t trust my “watchful waiting” skills. Nor indeed can these be utilised when the patient will see a different doctor next time
Continuity of care is vital, better triaging, and more time for complex cases.
Absolutely agree with all the article and comments so far. As someone who has studied medical sociology and as a patient who for many happy years – up to 2000 – had continuity of care and is now increasingly lost and anxious inthe desert of the present time, I wish & pray for the above changes – back to something like the old system. A consultant said to me, when I mentioned discussing something with my GP, ‘GPs know nothing!’ Rubbish: they understand the patients’ worries & concerns, they know the background stories, and can be a reassuring background presence when patients are required (by phone from a person unknown, usually an admin) to be called for tests and see one unknown ‘specialist’ after another.